- Research: Driving Progress Against Cancer
- Cancer: An Ongoing Public Health Challenge in the United States and Worldwide
- Variable Progress Among Cancer Types and Stages of Diagnosis
- Disparities in Progress for Certain U.S. Population Groups
- The Growing Burden of Cancer
- The Global Challenge of Cancer
- Funding Cancer Research: A Vital Investment
Cancer in 2021
In this section, you will learn:
- In the United States, the overall age-adjusted cancer death rates have decreased by 31 percent from 1991 to 2018, a reduction that translates into 3.2 million cancer deaths avoided.
- The decline in the overall cancer death rate is driven in large part by dramatic reductions in lung cancer and melanoma death rates.
- Progress has been made in understanding, and in some cases reducing, cancer health disparities since the 1990s. However, cancer still disproportionately affects racial and ethnic minorities and other underserved populations.
- Identifying the underlying causes of the rising incidence in certain early-onset cancers is critical for continued progress against cancer.
- While the Coronavirus Disease 2019 (COVID-19) has adversely affected all aspects of cancer research and care, scientists have responded in new and innovative ways to address the unique challenges posed by the pandemic.
- Robust and sustained cancer research funding is a vital investment for the U.S. economy.
Research: Driving Progress Against Cancer
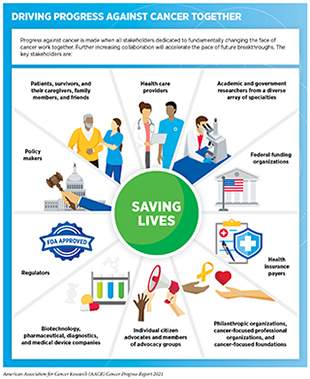
Advances in basic, clinical, translational, and population sciences are the catalysts that drive progress against cancer through improvements in prevention, detection, diagnosis, treatment, and survivorship. Research is also the driving force behind every new policy designed to improve public health. The collective impact of cancer research is felt through the numerous lives saved every year in the United States (U.S.) and, increasingly, across the globe (1)Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer Statistics, 2021. CA Cancer J Clin. Published online 2021.. Advances at each level of cancer care stem from years-long interdisciplinary collaborations among stakeholders across the medical research community (see sidebar on Driving Progress Against Cancer Together).
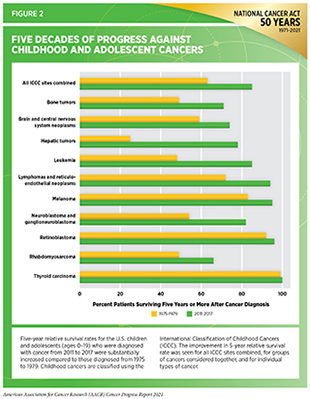
The year 2021 marks the 50th anniversary of the National Cancer Act that was signed into law by President Richard M. Nixon (2)Weinhouse S. National Cancer Act of 1971–an editorial. Cancer Res. Published online 1972.. The National Cancer Act placed a vital focus on the etiology, diagnosis, prevention, and treatment of cancers and, through multiple administrative and budgetary initiatives, enabled a cross-disciplinary approach to accelerate the pace of progress against cancer (2)Weinhouse S. National Cancer Act of 1971–an editorial. Cancer Res. Published online 1972.. Over the past five decades, the United States has made substantial progress in the fight against cancer, as underscored by the steadily declining overall cancer mortality rates. As a result, increasing numbers of children (ages 0-15), adolescents and young adults (AYA) (ages 15-39), and older adults (40 years and older) are surviving after a cancer diagnosis (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. The 5-year relative survival rate for all cancers combined has increased to 70 percent for people diagnosed between 2013 and 2017 from 49 percent for those diagnosed in the mid-1970s (4)Surveillance, Epidemiology, and End Results (SEER) Program.. This encouraging trend is also evident among U.S. children and adolescents (ages 0 to 19), for whom the 5-year relative survival rose from 63 percent to 84 percent over the same time interval (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15. (see Figure 2).
The extraordinary progress against cancer in the United States is further highlighted by a 31 percent decline in the age-adjusted overall cancer death rate from 1991 to 2018, which is the most recent year for which data are available. This includes a record 2.4 percent decline in the age-adjusted overall U.S. cancer death rate between 2017 and 2018, the largest reduction ever seen in a single year, and the second consecutive year in which a record decline in a single year was documented (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. The reduction in cancer death rates between 1991 and 2018 translates into 3.2 million cancer deaths avoided (4)Surveillance, Epidemiology, and End Results (SEER) Program..
The steady decline in overall cancer-related deaths in the United States in the past five decades can be attributed largely to the bench-to-bedside advances across the continuum of cancer science and medicine (see Supplemental Figure 1). Transformative discoveries, catalyzed by federal funding for cancer research, are rapidly culminating in improved prevention, early detection, diagnosis, and treatments for cancer. In this report, we highlight the advances made during the 12 months from August 1, 2020 to July 31, 2021. During this period, FDA approved 16 new anticancer treatments, three new cancer imaging agents, and two new cancer surgery guiding devices. Over these 12 months FDA also expanded the use of 11 previously approved anticancer therapeutics to treat additional cancer types (see Progress Across the Spectrum of Cancer Treatment). As we continue to make scientific and policy strides in cancer prevention, etiology, detection, diagnosis, treatment, and survivorship, we will seize the moment and maintain the momentum of progress against cancer.
Harnessing Cross-disciplinary Collaborations to Improve Outcomes for Patients with Metastatic Cancers
The steady decrease in overall cancer-related deaths in the United States since the signing of the National Cancer Act in 1971 is driven primarily by progress against the five most common cancer types: breast cancer, prostate cancer, lung cancer, colorectal cancer, and melanoma (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. Of these cancer types, progress made against various subtypes of lung cancer, including those that have spread to other parts of the body (metastatic), offers instructive insights into the collective and positive impact of cross-disciplinary approaches to basic, translational, and clinical research, population sciences, and public policy in combating this devastating disease.
Public Education and Policy Driving Progress in Lung Cancer Prevention
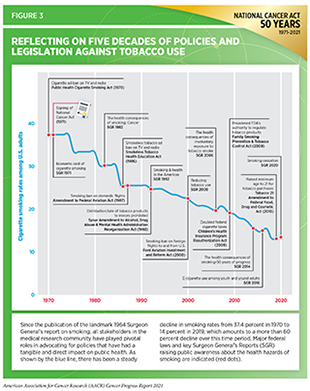
In the past five decades, major tobacco control policies have become laws at all levels of government (see Figure 3). These laws have changed social norms surrounding smoking (13)Secondhand Smoke Exposure and Cardiovascular Effects: Making Sense of the Evidence.; 2010.; decreased the use of tobacco (14)Substance Abuse and Mental Health Services Administration. About the Synar Amendment and Program. 1992.(15)U.S. Food & Drug Administration.Tobacco 21. 2019 [updated 2021 Feb 22; cited 2021 Mar 5].; increased the financial cost of producing, distributing, and buying tobacco products (16)Henry BJ. Impact of tobacco-control legislation. Clin J Oncol Nurs. Published online 2013.; and raised the federal minimum age of sale of all tobacco products from 18 to 21 (also see Reducing Tobacco-related Illness Through Public Health Policy)(15)U.S. Food & Drug Administration.Tobacco 21. 2019 [updated 2021 Feb 22; cited 2021 Mar 5].. In parallel, multiple U.S. government agencies, including Centers for Disease Control and Prevention (CDC), Food and Drug Administration (FDA), National Cancer Institute (NCI), and National Institutes of Health (NIH), have deployed concerted and coordinated tobacco control strategies. These efforts are exemplified by some of the major initiatives that NCI undertook to reduce smoking among Americans:
- In 1988, the Community Intervention Trial for Smoking Cessation (COMMIT) provided persistent tobacco cessation messaging through community mobilization, and resulted in modest increases in cessation rates among light-to-moderate smokers (17)Glynn TJ, Shopland DR, Manley M, et al. Community intervention trial for smoking cessation (COMMIT): II. Changes in adult cigarette smoking prevalence. Am J Public Health. 1995;85[tooltip text="2" url="https://cancerres.aacrjournals.org/content/32/4/i" newwindow="true"]Weinhouse S. National Cancer Act of 1971–an editorial. Cancer Res. Published online 1972.(18)Glynn TJ, Shopland DR, Manley M, et al. Community intervention trial for smoking cessation (COMMIT): I. Cohort results from a four-year community intervention. Am J Public Health. 1995;85(2).;
- In 1991, the American Stop Smoking Intervention Study (ASSIST) deployed policy-based approaches to prevent and reduce tobacco use; 17 states that implemented ASSIST had a greater decrease in adult smoking prevalence than states that did not implement the intervention (19)Stillman FA, Hartman AM, Graubard BI, Gilpin EA, Murray DM, Gibson JT. Evaluation of the American Stop Smoking Intervention Study (ASSIST): A report of outcomes. J Natl Cancer Inst. 2003;95(22).; and
- In 2011, the State and Community Tobacco Control (SCTC) Research Initiative promoted innovative research that benefits state and community tobacco control efforts. Areas of research included secondhand smoking, tobacco tax and pricing, and tobacco industry marketing and promotion (20)Roeseler A, Meaney M, Riordan M, Solomon M, Herndon S, Hallett C. NCI’s state and community research initiative: A model for future tobacco control research. Tob Control. 2016;25..
The Smokefree.gov Initiative, created and managed by the Tobacco Control Research Branch of NCI, is currently in its 17th year and provides free and evidence-based assistance to smoking cessation through online and smart phone-based resources.
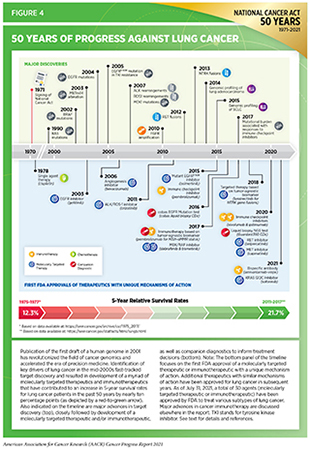
Implementation of nationwide public education campaigns, as well as comprehensive tobacco control policies, has resulted in a significant decrease in the U.S. smoking rates from 37.4 percent in 1971 to 14 percent in 2019 (12)Centers for Disease Control and Prevention. Current cigarette smoking among adults in the United States. 2020 [updated 2020 Dec 10; cited 2021 March 5].(21)Meza R, Jimenez-Mendoza E, Levy DT. Trends in Tobacco Use Among Adolescents by Grade, Sex, and Race, 1991-2019. JAMA Netw open. 2020;3(12):e2027465.(22)National Center for Chronic Disease Prevention and Health Promotion (US) Office on Smoking and Health. The health consequences of smoking—50 years of progress: a report of the Surgeon General. Atlanta (GA): Centers for Disease Control and Prevention (US); 2014.(23)Cornelius ME, Wang TW, Jamal A, Loretan CG, Neff LJ. Tobacco Product Use Among Adults — United States, 2019. MMWR Morb Mortal Wkly Rep. Published online 2020. (see Figure 3). As a result, far fewer Americans are dying from lung cancer today than did just two decades ago (24)Henley SJ, Ward EM, Scott S, et al. Annual Report to the Nation on the Status of Cancer, part I: National cancer statistics. Cancer. Published online 2020:2225-2249.. During 2011 – 2017, the latest time period for which such data are available, nearly 10 percent more Americans were surviving five years or longer after lung cancer diagnosis compared to 1975 – 1977(3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. The sharp decline in lung cancer deaths in the last two decades also parallels the unprecedented pace of discoveries in basic and translational research leading to clinical breakthroughs against lung cancer.
Landmark Discoveries Fueling Advances in Lung Cancer Diagnosis and Treatment
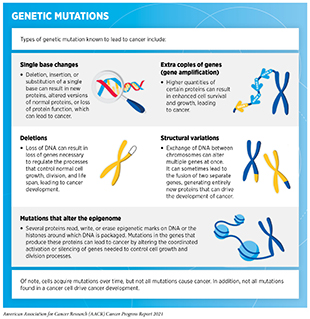
Like most other cancers, mechanisms underlying the onset and progression of lung cancer are complex and heterogeneous (25)Gridelli C, Rossi A, Carbone DP, et al. Non-small-cell lung cancer. Nat Rev Dis Prim. Published online 2015.. Breakthrough discoveries decoding the initiation and progression of lung cancer have provided valuable insights into early detection and treatment. Early detection among individuals who are at a high risk of developing lung cancer, primarily due to tobacco use, is saving lives (see Screening for Early Detection)(26)Jonas DE, Reuland DS, Reddy SM, et al. Screening for Lung Cancer With Low-Dose Computed Tomography: Updated Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA. 2021;325(10):971-987.. Basic research discoveries have taught us that lung cancers are driven by alterations, also referred to as mutations (see sidebar on Genetic Mutations), in several key genes, such as the oncogenic rat sarcoma (RAS)(27)Suzuki Y, Orita M, Shiraishi M, Hayashi K, Sekiya T. Detection of ras gene mutations in human lung cancers by single-strand conformation polymorphism analysis of polymerase chain reaction products. Oncogene. 1990;5:1037–43.(28)Graziano SL, Gamble GP, Newman NB, et al. Prognostic significance of K-ras codon 12 mutations in patients with resected stage I and II non-small-cell lung cancer. J Clin Oncol. Published online 1999.(29)Mitsudomi T, Viallet J, Mulshine JL, Linnoila RI, Minna JD, Gazdar AF. Mutations of ras genes distinguish a subset of non-small-cell lung cancer cell lines from small-cell lung cancer cell lines. Oncogene. Published online 1991.(30)Nelson MA, Wymer J, Clements N. Detection of K-ras gene mutations in non-neoplastic lung tissue and lung cancers. Cancer Lett. Published online 1996.(31)Riely GJ, Marks J, Pao W. KRAS mutations in non-small cell lung cancer. In: Proceedings of the American Thoracic Society. ; 2009.(32)Ding L, Getz G, Wheeler DA, et al. Somatic mutations affect key pathways in lung adenocarcinoma. Nature. Published online 2008., Epidermal Growth Factor Receptor (EGFR)(33)Lynch TJ, Bell DW, Sordella R, et al. Activating Mutations in the Epidermal Growth Factor Receptor Underlying Responsiveness of Non–Small-Cell Lung Cancer to Gefitinib. N Engl J Med. Published online 2004.(34)Paez JG, Jänne PA, Lee JC, et al. EGFR mutations in lung, cancer: Correlation with clinical response to gefitinib therapy. Science (80- ). Published online 2004.(35)Kobayashi S, Boggon TJ, Dayaram T, et al. EGFR Mutation and Resistance of Non–Small-Cell Lung Cancer to Gefitinib . N Engl J Med. Published online 2005., Fibroblast Growth Factor Receptor (FGFR)(36)Weiss J, Sos ML, Seidel D, et al. Frequent and focal FGFR1 amplification associates with therapeutically tractable FGFR1 dependency in squamous cell lung cancer. Sci Transl Med. Published online 2010., Anaplastic Lymphoma Kinase (ALK)(37)Soda M, Choi YL, Enomoto M, et al. Identification of the transforming EML4-ALK fusion gene in non-small-cell lung cancer. Nature. Published online 2007.(38)Lipson D, Capelletti M, Yelensky R, et al. Identification of new ALK and RET gene fusions from colorectal and lung cancer biopsies. Nat Med. Published online 2012., c-ros oncogene 1 (ROS1)(39)Rikova K, Guo A, Zeng Q, et al. Global Survey of Phosphotyrosine Signaling Identifies Oncogenic Kinases in Lung Cancer. Cell. Published online 2007., Rearranged during Transfection (RET)(38)Lipson D, Capelletti M, Yelensky R, et al. Identification of new ALK and RET gene fusions from colorectal and lung cancer biopsies. Nat Med. Published online 2012.(40)Ju YS, Lee WC, Shin JY, et al. A transforming KIF5B and RET gene fusion in lung adenocarcinoma revealed from whole-genome and transcriptome sequencing. Genome Res. Published online 2012.(41)Kohno T, Ichikawa H, Totoki Y, et al. KIF5B-RET fusions in lung adenocarcinoma. Nat Med. Published online 2012.(42)Takeuchi K, Soda M, Togashi Y, et al. RET, ROS1 and ALK fusions in lung cancer. Nat Med. Published online 2012., Mesenchymal-Epithelial Transition factor (MET)(43)Wolf J, Seto T, Han J-Y, et al. Capmatinib in MET Exon 14–Mutated or MET -Amplified Non–Small-Cell Lung Cancer . N Engl J Med. 2020;383(10).(44)Santarpia M, Massafra M, Gebbia V, et al. A narrative review of MET inhibitors in non-small cell lung cancer with MET exon 14 skipping mutations. Transl Lung Cancer Res. 2021;10(3)., and Neurotrophic Tropomyosin Receptor Kinase (NTRK)(45)Vaishnavi A, Capelletti M, Le AT, et al. Oncogenic and drug-sensitive NTRK1 rearrangements in lung cancer. Nat Med. Published online 2013., among others. Alterations in these genes allow cancer cells to grow unchecked and evade cell death (46)Hanahan D, Weinberg RA. Hallmarks of cancer: The next generation. Cell. 2011;144(5).. Molecular characterization of the lung cancer genome has highlighted the diversity of genetic alterations present in the disease. These findings have provided important mechanistic insights into lung cancer biology and have fueled the development of a class of highly effective anticancer treatments known as molecularly targeted therapeutics.
In addition to the discoveries that uncovered the genetic and epigenetic underpinnings of lung cancer, decades of basic research in immunology have led to the identification of immune checkpoint proteins, including PD-1 and CTLA-4, that function as “brakes” on T cell activation and can help cancer cells evade destruction by the immune system (47)Nicholson LB. The immune system. Essays Biochem. 2016;60(3).(48)Buchbinder EI, Desai A. CTLA-4 and PD-1 pathways similarities, differences, and implications of their inhibition. Am J Clin Oncol Cancer Clin Trials. 2016;39(1).(49)Reckamp KL. Advances in immunotherapy for non–small cell lung cancer. Clin Adv Hematol Oncol. 2015;13:847–53. (see Releasing the Brakes on Immune System). This knowledge has resulted in the development of a class of immunotherapeutics, known as the immune checkpoint inhibitors, that relieve suppression of a patient’s immune system by cancer cells, thus allowing T cells to attack and eliminate cancer cells (50)Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer. 2012;12(4).. Treatment with immune checkpoint inhibitors has yielded remarkably durable responses for many patients with lung cancer (51)Qiu Z, Chen Z, Zhang C, Zhong W. Achievements and futures of immune checkpoint inhibitors in non-small cell lung cancer. Exp Hematol Oncol. 2019;8(1)..
The transformation in the lung cancer treatment landscape has been staggering during just the past decade. In 2010, there were only three FDA-approved molecularly targeted therapeutics—gefitinib (Iressa) and erlotinib (Tarceva) directed against just one molecular target, EGFR, and bevacizumab (Avastin), an angiogenesis inhibitor—to treat patients with lung cancer (52)Yuan M, Huang LL, Chen JH, Wu J, Xu Q. The emerging treatment landscape of targeted therapy in non-small-cell lung cancer. Signal Transduct Target Ther. Published online 2019.. As of July 31, 2021, 30 agents—molecularly targeted therapeutics and immune checkpoint inhibitors—have been approved by FDA to treat various subtypes of lung cancer (52)Yuan M, Huang LL, Chen JH, Wu J, Xu Q. The emerging treatment landscape of targeted therapy in non-small-cell lung cancer. Signal Transduct Target Ther. Published online 2019.(53)Da Cunha Santos G, Shepherd FA, Tsao MS. EGFR mutations and lung cancer. Annu Rev Pathol Mech Dis. 2011;6:49-69.(54)Iams WT, Porter J, Horn L. Immunotherapeutic approaches for small-cell lung cancer. Nat Rev Clin Oncol. Published online 2020. (see Figure 4). These new treatment options include additional molecularly targeted therapeutics against EGFR and its specific mutated forms, as well as targeted therapeutics against a myriad of additional molecules such as ALK, ROS, MET, RET, NTRK, and one variant of the historically intractable target KRAS (G12C).
Identification of cellular and molecular alterations that drive lung cancer development has led to the discovery of numerous biomarkers (see Figure 4), which are foundational to the development of companion diagnostic tests for cancer treatment. Companion diagnostic tests guide treatment decisions by determining whether specific cellular or molecular characteristics, such as genetic alterations, are present in a patient’s lung cancer (55)Fan YS. Companion diagnostic testing for targeted cancer therapies: An overview. Genet Test Mol Biomarkers. Published online 2013.. In 2020, FDA approved the first companion diagnostic test that combines two cutting-edge technologies, known as next-generation sequencing and liquid biopsy, to identify cancer-driving alterations in the blood derived from patients with non–small cell lung cancer (NSCLC) to decide what treatment may be most effective (56)Gupta R, Othman T, Chen C, Sandhu J, Ouyang C, Fakih M. Guardant360 Circulating Tumor DNA Assay Is Concordant with FoundationOne Next‐Generation Sequencing in Detecting Actionable Driver Mutations in Anti‐EGFR Naive Metastatic Colorectal Cancer. Oncologist.
Rapid advances in the field of molecularly targeted therapeutics and immunotherapeutics have improved the outcomes for patients with several cancer types beyond lung cancer. As one example, progress made against metastatic lung cancer has been mirrored by equally impressive advances against metastatic melanoma, the deadliest form of skin cancer. Research-driven discoveries have contributed to the development and approval of innovative new treatments for patients with melanoma (see Figure 5), leading to a steady decline in the melanoma death rate, which has fallen by more than 5 percent every year from 2013 to 2018, the most recent year for which such data are available (4)Surveillance, Epidemiology, and End Results (SEER) Program.(57)Islami F, Ward EM, Sung H, et al. Annual Report to the Nation on the Status of Cancer, Part 1: National Cancer Statistics. JNCI J Natl Cancer Inst. Published online July 2021..
Cancer: An Ongoing Public Health Challenge in the United States and Worldwide
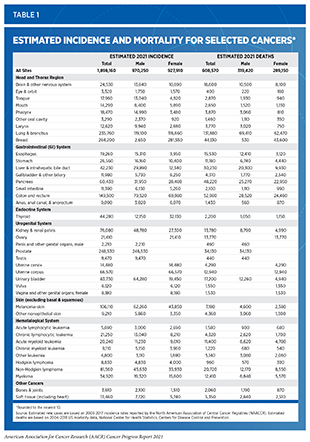
Despite the unprecedented progress against cancer since the signing of the National Cancer Act (2)Weinhouse S. National Cancer Act of 1971–an editorial. Cancer Res. Published online 1972., the disease continues to be a leading cause of death in the United States and around the world (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.(61)Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. Published online 2021.. In the United States, an estimated 1,898,160 new cancer cases and 608,570 deaths from the disease are projected in 2021 alone (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15. (Table 1). These numbers translate into approximately 18 new patients diagnosed with cancer, and nearly six patients dying from cancer, every five minutes.
Since its onset in early 2020, the Coronavirus Disease 19 (COVID-19) pandemic has further hampered our advances against cancer by negatively impacting all aspects of cancer science and medicine. While the full impact of COVID-19 on cancer research and care is yet to be determined, evidence for adverse effects of the pandemic across the continuum of cancer science and medicine is rapidly accruing. These adverse effects include decreased productivity and lost career opportunities among cancer researchers, in particular, among early-stage, minority, and female investigators because of the closures of and restricted access to research institutes (62)Caruso C. Covid-19 hits cancer research funding. Cancer Discov. Published online 2020.; refocused expertise and resources by some cancer researchers to study severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which causes COVID-19 (63)Zon L, Gomes AP, Cance WG, et al. Impact of COVID-19 Pandemic on Cancer Research. Cancer Cell. 2020;38(5).; considerably reduced research funding by nonprofit cancer societies (62)Caruso C. Covid-19 hits cancer research funding. Cancer Discov. Published online 2020., which typically contribute up to 50 percent of all cancer research funding in the United States (64)Kamath SD, Kircher SM, Benson AB. HSR19-094: A Comparison of Cancer Burden and Funding From the National Cancer Institute and Nonprofit Organizations Reveals Disparities in the Distribution of Funding Across Cancer Types. J Natl Compr Cancer Netw. 2019;17; substantially reallocated financial resources by many health care systems away from cancer care to address the challenges imposed by the COVID-19 pandemic (65)Birkmeyer JD, Barnato A, Birkmeyer N, Bessler R, Skinner J. The impact of the COVID-19 pandemic on hospital admissions in the United States. Health Aff. 2020;39(11).(66)Patt D, Gordan L, Diaz M, et al. Impact of COVID-19 on Cancer Care: How the Pandemic Is Delaying Cancer Diagnosis and Treatment for American Seniors. JCO Clin Cancer Informatics. 2020;(4):1059-1071.(67)American Hospital Association. Hospitals and health systems face unprecedented financial pressures due to COVID-19. 2020 May [cited 2021 Aug 9].; disruption in cancer screening, diagnosis, and treatment; and a significant decline in clinical trial enrollment and conduct (63)Zon L, Gomes AP, Cance WG, et al. Impact of COVID-19 Pandemic on Cancer Research. Cancer Cell. 2020;38(5).(68)Lamont EB, Diamond SS, Katriel RG, et al. Trends in Oncology Clinical Trials Launched before and during the COVID-19 Pandemic. JAMA Netw Open. 2021;4(1):2020-2022.(69)Marcum M, Kurtzweil N, Vollmer C, et al. COVID-19 pandemic and impact on cancer clinical trials: An academic medical center perspective. Cancer Med. 2020;9(17)..
There are also serious concerns about the higher burden of COVID-19 for patients with cancer. Multiple studies indicate that cancer patients are at a greater risk of COVID-19 infection and mortality (70)Ribas A, Sengupta R, Locke T, et al. Priority covid-19 vaccination for patients with cancer while vaccine supply is limited. Cancer Discov. 2021;11(2):233-236.(71)Sng CCT, Wong YNS, Wu A, et al. Cancer History and Systemic Anti-Cancer Therapy Independently Predict COVID-19 Mortality: A UK Tertiary Hospital Experience. Front Oncol. 2020;10(November):1-8.(72)Cattaneo C, Daffini R, Pagani C, et al. Clinical characteristics and risk factors for mortality in hematologic patients affected by COVID-19. Cancer. 2020;126(23):5069-5076.(73)Meng Y, Meng Y, Lu W, et al. Cancer history is an independent risk factor for mortality in hospitalized COVID-19 patients: A propensity score-matched analysis. J Hematol Oncol. 2020;13(1).(74)Mehta V, Goel S, Kabarriti R, et al. Case Fatality Rate of Cancer Patients with COVID-19 in a New York Hospital System. Cancer Discov. 2020;10(7).(75)Rüthrich MM, Giessen-Jung C, Borgmann S, et al. COVID-19 in cancer patients: clinical characteristics and outcome—an analysis of the LEOSS registry. Ann Hematol. Published online 2020.(76)Lunski MJ, Burton J, Tawagi K, et al. Multivariate mortality analyses in COVID-19: Comparing patients with cancer and patients without cancer in Louisiana. Cancer. 2021;127(2):266-274.(77)Tian J, Yuan X, Xiao J, et al. Clinical characteristics and risk factors associated with COVID-19 disease severity in patients with cancer in Wuhan, China: a multicentre, retrospective, cohort study. Lancet Oncol. 2020;21(7):893-903.(78)Dai M, Liu D, Liu M, et al. Patients with cancer appear more vulnerable to SARS-CoV-2: A multicenter study during the COVID-19 outbreak. Cancer Discov. 2020;10(6).(79)Ludi Yang et al. Effects of cancer on patients with COVID-19: a systematic review and meta-analysis of 63,019 participants. Cancer Biol Med. 2021;18(1):298-307.. This risk is the highest for patients with lung cancer and hematological malignancies and among patients from certain underserved population groups (79)Ludi Yang et al. Effects of cancer on patients with COVID-19: a systematic review and meta-analysis of 63,019 participants. Cancer Biol Med. 2021;18(1):298-307.(80)Wang QQ, Berger NA, Xu R. Analyses of Risk, Racial Disparity, and Outcomes among US Patients with Cancer and COVID-19 Infection. JAMA Oncol. 2020;44106:1-8.(81)Garassino MC, Whisenant JG, Huang LC, et al. COVID-19 in patients with thoracic malignancies (TERAVOLT): first results of an international, registry-based, cohort study. Lancet Oncol. 2020;21(7).(82)Lara OD, O’Cearbhaill RE, Smith MJ, et al. COVID-19 outcomes of patients with gynecologic cancer in New York City. Cancer. 2020;126(19).(83)Van Haren RM, Delman AM, Turner KM, et al. Impact of the COVID-19 Pandemic on Lung Cancer Screening Program and Subsequent Lung Cancer. J Am Coll Surg. Published online 2020.(84)Xu Y, Liu H, Hu K, Wang M. Clinical management of lung cancer patients during the outbreak of 2019 novel coronavirus disease (Covid-19). Chinese J Lung Cancer. Published online 2020.(85)Hultcrantz M, Richter J, Rosenbaum CA, et al. COVID-19 Infections and Clinical Outcomes in Patients with Multiple Myeloma in New York City: A Cohort Study from Five Academic Centers. Blood Cancer Discov. 2020;1(3).(86)Williamson EJ, Walker AJ, Bhaskaran K, et al. Factors associated with COVID-19-related death using OpenSAFELY. Nature. 2020;584(7821).(87)Wang QQ, Berger NA, Xu R. When hematologic malignancies meet COVID-19 in the United States: Infections, death and disparities. Blood Rev. Published online 2020. (see sidebar on COVID-19 in Patients With Cancer). A comprehensive overview of the impact of COVID-19 on cancer research and patient care will be presented in a separate AACR report to be released in early 2022.
Variable Progress Among Types of Cancer and Stages of Diagnosis
Cancer is a heterogeneous disease, and because of that, progress against cancer has not been uniform across different types of cancer or for all stages of a given cancer type (88)Elmore LW, Greer SF, Daniels EC, et al. Blueprint for cancer research: Critical gaps and opportunities. CA Cancer J Clin. Published online 2020.(89)Zugazagoitia J, Guedes C, Ponce S, Ferrer I, Molina-Pinelo S, Paz-Ares L. Current Challenges in Cancer Treatment. Clin Ther. Published online 2016..
A key indicator of these challenges is the 5-year relative survival rate, which varies widely depending on the cancer type and stage (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. For example, there are striking differences between 5-year relative survival rates for breast (female) cancer and melanoma compared to pancreatic and liver cancers. For those diagnosed between 2011 and 2017, the most recent time frame for which such data are reported, 90 percent of patients diagnosed with breast cancer and 93 percent of those diagnosed with melanoma were surviving five years or more. In comparison, during the same time period, only 11 percent of patients diagnosed with pancreatic cancer and 20 percent of patients diagnosed with liver cancer survived five years or more (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15..
Five-year relative survival rates also differ drastically for patients with a given type of cancer, depending on how advanced their cancer is at the time of diagnosis. As an example, women who are diagnosed with breast cancer that is still confined entirely to breast tissue (i.e., early-stage or localized breast cancer) have a 99 percent 5-year relative survival rate. By contrast, only 29 percent of women who are diagnosed when breast cancer has already spread to other organs and tissues in the body (i.e., late-stage or distant breast cancer) live five years or more after diagnosis (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. Similarly, 5-year relative survival rates for men diagnosed with localized versus distant prostate cancer are greater than 99 percent versus 31 percent, respectively (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.. These statistics point to the critical need of developing new, effective, and when possible, minimally invasive tests (see Figure 13) that can detect cancer at the earliest possible stage, when treatments are more likely to be curative. Furthermore, concerted efforts to increase the uptake of routine cancer screening among eligible populations (see Screening for Early Detection) and to enhance the adoption of preventive measures that can reduce the risk of cancer (see Preventing Cancer: Identifying Risk Factors) can substantially reduce the burden of cancer in coming years.
Disparities in Progress for Certain U.S. Population Groups
Cancer affects all people, but certain segments of the U.S. population with social, environmental, and economic disadvantages experience a disproportionate burden of cancer (see sidebar on Which U.S. Population Groups Experience Cancer Health Disparities?).
The NCI defines cancer health disparities as adverse differences in cancer experienced by certain segments of the U.S. population such as the number of new cases and deaths, cancer-related health complications, quality of life after cancer treatment, financial burden, screening rates, and stage at diagnosis (see sidebar on U.S. Cancer Health Disparities).
Considerable progress has been made in documenting cancer disparities over the past two decades, which in turn has informed policies to address these inequalities (see Addressing Cancer Health Disparities) (91)Sengupta R, Honey K. AACR Cancer Disparities Progress Report 2020 : Achieving the Bold Vision of Health Equity for Racial and Ethnic Minorities and Other Underserved Populations . Cancer Epidemiol Biomarkers Prev. Published online 2020.(98)Zavala VA, Bracci PM, Carethers JM, et al. Cancer health disparities in racial/ethnic minorities in the United States. Br J Cancer. 2021;124(2):315-332.(99)Miller JW, Plescia M, Ekwueme DU. Public health national approach to reducing breast and cervical cancer disparities. Cancer. Published online 2014.(100)Adler NE, Newman K. Socioeconomic disparities in health: Pathways and policies. Health Aff. Published online 2002.. There are also some encouraging signs of narrowing disparities, as evidenced by declining cancer incidence and mortality rates among underserved population groups. During 2008–2017, the most recent period for which such data are available, the overall cancer incidence rates decreased faster among African American males (2.3 percent per year) compared to white males (1.7 percent per year). Cancer mortality also declined faster among African Americans than whites for both males (2.7 percent versus 1.7 percent per year) and females (1.6 percent versus 1.3 percent per year) (92)American Cancer Society. Cancer Facts and Figures for African Americans 2019-2021. Am Cancer Soc. 2021.. Despite these improvements, the burden of cancer is still substantially higher for racial and ethnic minorities and other underserved populations (91)Sengupta R, Honey K. AACR Cancer Disparities Progress Report 2020 : Achieving the Bold Vision of Health Equity for Racial and Ethnic Minorities and Other Underserved Populations . Cancer Epidemiol Biomarkers Prev. Published online 2020.(98)Zavala VA, Bracci PM, Carethers JM, et al. Cancer health disparities in racial/ethnic minorities in the United States. Br J Cancer. 2021;124(2):315-332.(101)Freedman JA, Abo M Al, Allen TA, Piwarski SA, Wegermann K, Patierno SR. Biological Aspects of Cancer Health Disparities. Annu Rev Med. Published online 2021.(102)Newman LA. Cascading Consequences of Systemic Racism on Public Health. Ann Surg. Published online 2021.. Unfortunately, the COVID-19 pandemic has further disrupted the progress made against cancer disparities (80)Wang QQ, Berger NA, Xu R. Analyses of Risk, Racial Disparity, and Outcomes among US Patients with Cancer and COVID-19 Infection. JAMA Oncol. 2020;44106:1-8..

Cancer health disparities experienced by underserved populations pose significant challenges, with long-term societal and economic ramifications for individuals and the entire nation. It is critical that all stakeholders in the medical research community work together to identify and eliminate the structural and systemic injustices that prevent health equity for the underserved groups of the U.S. population. The AACR Cancer Disparities Progress Report 2020 summarizes current knowledge of the complexities that we must overcome to address cancer health disparities and identifies key areas where progress can, and must, be made (91)Sengupta R, Honey K. AACR Cancer Disparities Progress Report 2020 : Achieving the Bold Vision of Health Equity for Racial and Ethnic Minorities and Other Underserved Populations . Cancer Epidemiol Biomarkers Prev. Published online 2020. (see sidebar on Why Do U.S. Cancer Health Disparities Exist?).
The Growing Burden of Cancer
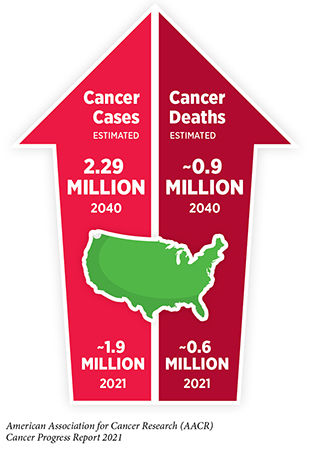
The burden of cancer is growing rapidly in the United States and worldwide. According to the latest estimates from the World Health Organization (WHO), cancer was the first or second leading cause of death before the age of 70 in 112 out of 183 countries in 2019 (103)WHO report on cancer: setting priorities, investing wisely and providing care for all. Geneva: World Health Organization; 2020. Licence: CC BY-NC-SA 3.0 IGO.. In the United States, researchers estimate that the number of new cancer cases will exceed 2.2 million and the number of cancer deaths will reach nearly 900,000 by the year 2040 (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.(61)Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. Published online 2021.. Overcoming the burdens posed by cancer necessitates developing and implementing effective strategies across the continuum of cancer research and care.
The anticipated sharp increases in the number of new cancer cases and cancer deaths reflect both the projected overall population growth and the expected increase in the population that is age 65 or older. Cancer is primarily a disease of aging. Individuals who are age 65 and older account for 54 percent of new cancer diagnoses (4)Surveillance, Epidemiology, and End Results (SEER) Program., and this population in the United States is expected to grow from 56 million in 2020 to 82.7 million in 2045 (104)2017 National Population Projections Datasets [Internet]. U.S. Census Bureau. Washington, DC. 2017..
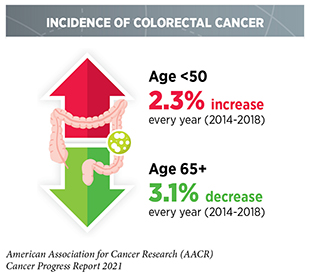
Substantial progress has been made toward reducing cancer incidence in the United States; new cancer cases have declined 13 percent from their peak in 1992 to 2018, the year for which the most recent data are reported (4)Surveillance, Epidemiology, and End Results (SEER) Program.. However, overall cancer incidence has been rising among the AYA population (ages 15 to 39), which has seen nearly a 30 percent increase in cancer incidence from 1973 to 2015 (105)Scott AR, Stoltzfus KC, Tchelebi LT, et al. Trends in Cancer Incidence in US Adolescents and Young Adults, 1973-2015. JAMA Netw open. 2020;3(12):e2027738.. In addition, the incidence of certain cancer types is on the rise specifically among people younger than 50 (106)Siegel RL, Torre LA, Soerjomataram I, et al. Global patterns and trends in colorectal cancer incidence in young adults. Gut. 2019;68(12):2179-2185.(107)A B, F S, R B. Prostate Cancer in Young Men: An Emerging Young Adult and Older Adolescent Challenge. Cancer. 2020;126(1).. As one example, a recent study has reported that new cases of esophageal cancer increased among people younger than 50 nearly three percent every year between 1975 and 2015 (108)Codipilly DC, Sawas T, Dhaliwal L, et al. Epidemiology and Outcomes of Young-Onset Esophageal Adenocarcinoma: An Analysis from a Population-Based Database. Cancer Epidemiol Biomarkers Prev. Published online December 2020.. This is especially concerning because esophageal cancers among this population were detected at more advanced stages (84.9 percent) compared to those detected among patients older than 50 (67.3 percent, respectively). Another alarming trend is that new cases of colorectal cancer among individuals younger than 50 have been rising since 2007, and the increases are especially high among American Indians/Alaska Natives and non-Hispanic whites (109)Siegel RL, Miller KD, Goding Sauer A, et al. Colorectal cancer statistics, 2020. CA Cancer J Clin. 2020;70(3):145-164.. These trends of early-onset colorectal cancer have prompted U.S. Preventive Services Task Force (USPSTF), as well as some cancer-focused professional societies and organizations, to update existing guidelines recommending that screening for colorectal cancer start at an earlier age (see sidebar on Consensus Cancer Screening Recommendations for Average-risk Individuals).

The Global Challenge of Cancer
Beyond the United States, the burden of cancer is growing rapidly across the globe. According to the latest estimates from World Health Organization (WHO), cancer was the first or second leading cause of death before the age of 70 in 112 out of 183 countries in 2019 and accounted for nearly 10 million deaths worldwide in 2020 (61)Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. Published online 2021.. Notably, the global burden of cancer is predicted to rise significantly in the coming decades unless new and more effective approaches to cancer prevention, early detection, and treatment are developed and successfully implemented across the globe. The estimated increase in the global burden of cancer will be fueled by overall population growth and expansion in the segment of the world’s population most likely to develop cancer, i.e., those age 65 and older.
Cancer health disparities around the world are highlighted by the widely different cancer incidence and mortality rates across regions. As an example, low- and middle-income countries (LMICs) experienced a disproportionately higher burden of cancer and, in fact, shouldered 65 percent of all global cancer deaths in 2020, even though only 56 percent of new cancer cases occurred in these countries (110)Gopal S, Sharpless NE. Cancer as a Global Health Priority. JAMA. Published online August 2021. (see sidebar on Cancer: A Global Public Health Challenge).
The global disparities in the cancer burden largely reflect differences in exposure to risk factors as well as the barriers to high-quality cancer prevention and early detection in countries with limited resources. For example, it is estimated that the implementation of effective vaccination intervention will lead to the near elimination of HPV-related cervical cancer, in highly developed countries, such as Australia by the end of this decade (114)Hall MT, Simms KT, Lew J Bin, et al. The projected timeframe until cervical cancer elimination in Australia: a modelling study. Lancet Public Heal. 2019;4(1).. However, most low-income countries with high cervical cancer incidence will not achieve this target even by the end of this century (115)Brisson M, Kim JJ, Canfell K, et al. Impact of HPV vaccination and cervical screening on cervical cancer elimination: a comparative modelling analysis in 78 low-income and lower-middle-income countries. Lancet. 2020;395(10224).. In addition, low-income countries have had little to no access to the numerous cutting-edge diagnostic and anticancer therapeutic agents that have been approved by the Food and Drug Administration (FDA) in the United States. One area in which progress is urgently needed is in addressing the disparities in the conduct of cancer clinical trials which are vital for the development of new anticancer therapeutics. A recent analysis of contemporary cancer clinical trials across the globe showed that only eight percent of such studies were led by LMICs (116)Wells JC, Sharma S, Del Paggio JC, et al. An Analysis of Contemporary Oncology Randomized Clinical Trials from Low/Middle-Income vs High-Income Countries. JAMA Oncol. 2021;7(3).. These inequities limit our ability to reduce the global burden and suffering due to cancer.
Given the profound adverse impact of cancer on public health worldwide, it is imperative that the international biomedical research community work together to drive down cancer incidence and mortality and mitigate the global cancer inequities. In this regard, NCI established the Center for Global Health 10 years ago. The priorities of the center include supporting innovative, impactful research that addresses key scientific issues in global cancer control; supporting global cancer research training, particularly in LMICs, which enables global scientific collaboration; and promoting the integration of current scientific knowledge while engaging NCI with other key partners in global cancer control (118)American Cancer Society Cancer Action Network. The Costs of Cancer: 2020 Edition; 2020.. Notably, 13 percent of NCI’s extramural support in 2020 included international components, compared to only nine percent in 2010, while 32 percent of its international awards involved LMICs (110)Gopal S, Sharpless NE. Cancer as a Global Health Priority. JAMA. Published online August 2021.. Through a robust future scientific strategy that focuses on technologies for global cancer control, global cancer implementation science, global cancer health disparities, cancer clinical trials in LMICs, and understanding cancer etiology and biology through global collaborations, NCI aims to catalyze new discoveries to reduce the global incidence, morbidity, and mortality from cancer (110)Gopal S, Sharpless NE. Cancer as a Global Health Priority. JAMA. Published online August 2021..
Funding Cancer Research: A Vital Investment
The enormity of the challenges posed by cancer on the U.S. health and economy underscores the urgent need for more investments in cancer science and medicine. Investments in cancer research not only benefits all Americans through new discoveries that save lives, but also creates jobs that boost local economies across the nation.
The toll of cancer that is experienced by patients, their caregivers, friends, and family can never be quantified in dollar amounts. It is possible, however, to estimate the direct and indirect economic impact of cancer on the society as a whole. Cancer patients in the United States paid $5.6 billion out of pocket for cancer treatments in 2018 (118)American Cancer Society Cancer Action Network. The Costs of Cancer: 2020 Edition.; 2020., which is nearly the same as the total $6 billion NCI funding for cancer research that year (119)By the Numbers: NCI Budget Breakdown, FY 2018. Cancer Discov. Published online 2019.. Furthermore, an estimated $200.7 billion of total U.S. health care was spent on cancer-related health care in 2020 (120)Mariotto AB, Enewold L, Zhao J, Zeruto CA, Robin Yabroff K. Medical care costs associated with cancer survivorship in the United States. Cancer Epidemiol Biomarkers Prev. Published online 2020.. That number is projected to increase to $245.6 billion by 2030, which amounts to a 22.4 percent increase. These costs do not reflect the additional indirect economic burden weathered by the patients and their caregivers in lost earnings, and by employers in lost productivity (121)Zafar SY. Financial Toxicity of Cancer Care: It’s Time to Intervene. J Natl Cancer Inst. Published online 2016.. In addition, these financial burdens of cancer collectively contribute to cancer health disparities (121)Zafar SY. Financial Toxicity of Cancer Care: It’s Time to Intervene. J Natl Cancer Inst. Published online 2016.. It is projected that the adverse impact of the COVID-19 pandemic on cancer screening, diagnosis, and treatment will compound the already enormous toll of cancer (3)American Cancer Society. American Cancer Society: Cancer Facts and Figures 2021. Atlanta Am Cancer Soc. Published online 2021:13-15.(122)Rosenbaum L. The Untold Toll — The Pandemic’s Effects on Patients without Covid-19. N Engl J Med. Published online 2020..
The year 2021 marks the 50th anniversary of the National Cancer Act that was signed into law by President Richard Nixon (2)Weinhouse S. National Cancer Act of 1971–an editorial. Cancer Res. Published online 1972.. The National Cancer Act has catalyzed research across the continuum of cancer science and medicine. This year also marks the 20th anniversary of the publication of the human genome (123)Lander ES, Linton LM, Birren B, et al. Initial sequencing and analysis of the human genome. Nature. Published online 2001., which has accelerated the development of precision medicine, and the 10th anniversary of the annual AACR Cancer Progress Report (124)American Association for Cancer Research. AACR Cancer Progress Report 2011: Transforming Patient Cancer Through Innovation., which has chronicled the remarkable progress against cancer over the past decade. The unprecedented advances, highlighted in the current report and the ten prior editions, underscore how cross-disciplinary research has been vital in accelerating the pace of scientific innovation and emphasize the importance of public education and advocacy in our progress against cancer (see Investing in a Healthier Future Through Research). Importantly, fundamental discoveries that have led to developing effective approaches to preventing, detecting, and treating cancer would not have been possible without the public funding of cancer research through NIH and NCI. Increasing in our investments now will ensure that we prevent cancer incidence, morbidity, and mortality in the years and decades to come. Therefore, it is imperative that Congress continue to increase its investment, in a consistent and predictable manner, in federal agencies, including NIH, NCI, FDA, CDC, and Department of Defense (DoD), that are essential for turning discovery science into lifesaving care for all (see The AACR Call to Action).